Since I have time on my hands before we even start round #2 of IVF I thought I should go back and double check all of my fertility billing against my EOB’s (explanation of benefits) from my insurance. This process left one Dr.’s office owing us $20 in over billed co-pays (not that $20 is going to make or break this process) and another glaring question of which came first the pre-auth or the script?
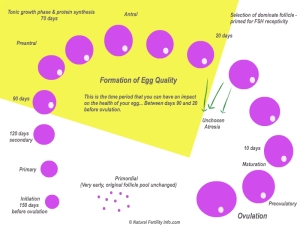
Lets reflect for a moment on Saizen. This is a human growth hormone that “allegedly” helps with egg quality. No debates on this one but rather the use of this drug in any type of fertility treatment is considered “off-label” and there for NOT covered by most insurance carriers. Off-label means “the medication is being used in a manner not specified in the FDA’s approved packaging label, or insert” – like Saizen for IVF but I digress, we had to pay $1500.00 out-of-pocket for our 2 vials of Saizen and I wanted to know if this went towards our deductible. I have since found out that my insurance deductibles and my Rx deductibles are NOT the same deductibles. As a matter of fact I had no idea that I had a deductible for Rx’s… This whole process has been so enlightening.
After 3 phone transfer’s and 20 minutes of round about dealing with folks I finally ended up in the “pre-authorization” department where I am now told that there is no request for a pre-auth on file and that’s why we had to pay out-of-pocket. Upon further detective questioning as I have found out that my Rx company does not like to tell you what you need to do to have a prescription covered they simply decline and say that it is not covered. A great example of this was an Rx that I had for the only round of IUI that we did. It was 10 pills but my Rx company turned it down because the script wasn’t written for a 30 day timeframe. How the hell am I suppose to know this? I also found out that my copays are different for 30/60/90 scripts and are much cheaper if purchase the 90 day supply with only one copay.
My Rx company will cover back dated claims up to 12 months if there is an approved pre-auth on file. Conceptions cant/wont put in a pre-auth request unless there is an “actual” script request… there was one in March… I am left wondering why this one doesn’t count.
So which comes first the pre-auth or the Rx? I now have a pharmacy calling me wanting to fill the new script but I cant talk to anyone at Rx company until Monday to see if the pre-auth has been requested.
Right now we aren’t doing anything different than we did the last time I had script filled for an IVF with Conceptions. Where is the pre-auth? We all know what happens when you do the same thing and expect a different result.
AND if this gets declined on the pre-auth front then it stays as an out-of-pocket expense with $0 going towards the deductible… so wrong in so many ways.